Let’s face it: Today, patients expect personalized, dynamic, convenient communication with their healthcare providers – just like they experience in other industries.
And, they deserve it.
EVERY PERSON will become a patient at some point in their lifetime – you, me, and the physicians and nurses who will care for us. Our health is the most important part of our being and communication is a critical component to improving care adherence.
So in short: We deserve it.
Unfortunately, the reality is that many patients still receive BASIC communication from their healthcare provider: robo texts, one-way messages with no personalization, limited response options, and more.
At Artera, we believe patients deserve BETTER communications, not BASIC.
And if you’re ready to deliver a world-class communication experience to your patients, you’ll want to keep reading.
Here are nine ways to go beyond basic texting to deliver better conversations and therefore, improve the patient experience and outcomes:
#1: Go Beyond Basic (One-Way or Two-Way) Texting With Conversational Messaging
It’s no surprise that more and more consumers are craving the simplicity, ease, and accessibility that texting can offer – and it’s clear healthcare leaders are taking note, as the industry now takes the lead for consumer SMS opt-ins in 2023 (55%). This is a notable increase from last year’s 49% – a 13% growth in healthcare-related opt-ins year over year.

But the days of basic texting in healthcare are gone. Robo texting, push notifications, and entering “1 to confirm” or replying “Y or N” are a thing of the past. We now know patients not only want to interact with a live human to get their questions answered, if needed, but they also want to text in their own words or emojis and engage in dynamic, real conversations with their care team.
Basic platforms that only support hard-coded “two-way” basic texting – with no NLU or live staff support – cannot live up to patient expectations today. So, if you know your patients aren’t basic, why would you treat them like they are by using basic texting? Basic patient messaging is robotic, predefined, and quite frankly – archaic. Your staff and your patients deserve an upgrade.
Artera’s conversational messaging technology helps healthcare providers have better conversations with patients. It allows health systems to automate patient communications using natural language and AI, while also producing personalized interactions that help maintain the human touch – ensuring a beautiful balance between AI and human inclusion.
Conversational messaging goes well beyond one-way automations and older two-way healthcare texting solutions, providing an experience similar to messaging friends or family – something that patients are looking for. For health systems, Artera reduces call volume and patient outreach with conversational messaging – among a number of other features – such as broadcast messaging, campaign messaging, AI-enabled texting, call-to-text, and language support.
#2: Think Beyond Appointment Reminders
A good patient communication strategy isn’t just about appointment reminders – it’s about so much more: closing gaps in the patient journey, delivering workflows, and guaranteeing that patients convert. It’s also about automating processes and improving staff efficiency.
Our very own Meg Aranow, Platform Evangelist at Artera and former CIO at Boston Medical Center, believes that there is so much more opportunity to engage with a patient beyond appointment reminders:
“Making sure patients come in for their visits – and are reminded at an appropriate cadence – is almost table stakes at this point. Now we’re going further and we’re starting to message patients after their visit to make sure that they’re doing the follow-up care, they’re refilling their prescriptions, and more – we can really start to see tangible outcomes if a patient is following through with their care now.”
That being said, most basic platforms in the market today provide limited functionality – likely just appointment reminders – to reach patients. This not only feels transactional in nature but does nothing to enable deeper connections with your patients. So, why limit your workflow to just appointment reminders?
The Artera platform goes well beyond just appointment reminders, supporting hundreds of workflows spanning the entire patient journey – everything from referrals to recalls, post-discharge, and more. This enables a more cohesive patient experience, engaging them across the entire care continuum – beyond just a single appointment instance.
#3: Minimize Message Fatigue by Integrating Vendors Across Your Tech Stack
Communication burnout, or “texting fatigue,” is a real thing. We all know how overwhelming digital communication and constant notifications can be – sometimes to the point where reading and responding all just seems like too much at once, so we ignore it.
According to a 2020 report exploring the effects of information overload and online conversation dynamics, researchers found that “over-exposure to information can suppress the likelihood of response by overloading users.” It’s no wonder the average American has a whopping 47 unread text messages and over 1,600 unopened emails at a given time.
For healthcare communications alone, this issue has spiraled out of control, with an abundance of technology systems, specialties, and providers who are all competing for attention from the same patients. Our research found that most health systems have over 11 digital health vendors that communicate independently with patients, leaving many patients feeling “over-messaged” and fatigued.
The real issue here is too many texts from too many numbers and vendors, totally uncoordinated. This is the result of using basic platforms, or closed systems, that do not integrate with other vendors – and are each being managed by various departments within the health system, meaning there is limited-to-no awareness of competing communication workflows or messaging backlogs.
This is where Artera Harmony – our open platform – can deliver a more cohesive experience, orchestrate patient communication by integrating a hospital’s digital vendors, manage communication workflows from multiple stakeholders, and deliver communication to patients in a single unified and cohesive communication thread. This streamlined approach helps minimize message overload and consolidates various channels for personalized care delivery.
#4: Deliver Text Messages via Long Code
Have you ever received a message from a random number, thought “Oh no, who is this? It’s probably spam,” and then immediately deleted it? We’ve all been there – and you may even be so inclined to go one step further and block the number, thinking you’re doing yourself a favor.

In reality, however, this could’ve very well been your healthcare provider texting you via a basic patient communication platform – one that sends communications from a 5-digit short code, not the hospital’s main line. Without that context, it’s easy to imagine just how many patients view these short-code messages as spam – a common mistake that ultimately lowers response rates significantly (short-code messages: 39.3% response rate).1 But, as a provider, how will you engage these patients if they don’t know who you are?
With the Artera platform, communications are sent via long code from the hospital-enabled phone number – a recognizable phone number that the patient may have even saved in their contact list. This not only means texts and calls don’t get ignored but it also improves overall response rates from patients (long code messages: 70.5% response rate).1
#5: Deploy an Omnichannel Strategy
As a patient, you deserve options, especially in terms of how you communicate with your healthcare provider. Let’s just say you don’t have a cellphone, or maybe you’re just not that into texting and prefer calling or emailing instead. While this may seem shocking to some in today’s world, nearly 1 out of 5 patients use landlines only (i.e. cannot receive text messages.)2 This number may very well be more than that, too – in fact, one Artera customer in the Southern U.S. found that 35% of their patients were using landlines only.

Despite a significant portion of patients who use landlines only, some basic platforms only offer text messaging and do not have interactive voice response (IVR). What this means is that you cannot reach those patients with landlines – meaning you cannot reach a significant portion of your patient population. Are you comfortable not reaching these patients? If not, do you have Call Center resources to call those patients manually?
With Artera, you don’t have to think through these challenges. As a complete omnichannel solution, Artera offers messaging in patients’ preferred channels, including Voice/IVR, email, or text – giving you the ability to reach and engage more patients on their preferred communications channel – even those with landlines.
#6: Personalize Your Messaging As Much as Possible
It’s likely that you’ve received impersonal text messages from a variety of industries before – mass texts that were shared with thousands of other people to try and get you to buy or attend something. And with no personalization or customization, the message just feels dull or spammy – like a robotic, transactional interaction.
For providers using a basic platform, this is all they have to offer, as the workflows are hard-coded and offer limited customization – versions can not be created for specific patient cohorts, locations, providers, and event types. As a health system, are all of your departments and staff willing to use a unified, standard message for patients? How will you deliver a great experience and increase engagement when each patient receives a standard message regardless of their condition?
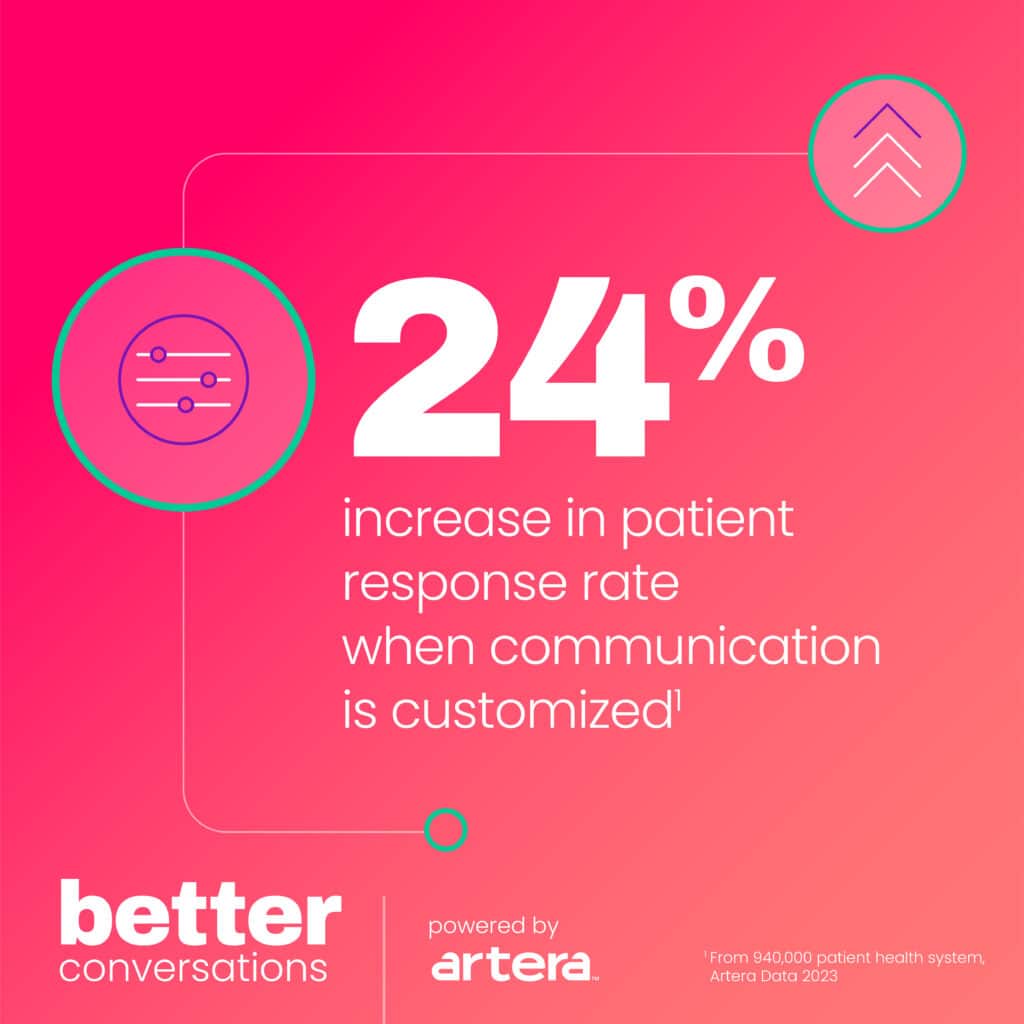
Artera offers tremendous, intuitive customization by location, event, provider workflows, and more. This means all of your various departments can create unique messages that resonate best with their unique patient population, leading to greater engagement. In fact, when communications like these are customized to the patient (e.g., patient name, location, and/or provider), there is a 24% increase in patient response rate.5
#7: Integrate Your Staff for Live Dialogue, When Needed
Imagine this: you’re busy at work and have limited time to look at your phone, but are texting an important question to your provider before an upcoming appointment. You end up getting back, “This line is not monitored.” You have two options: call in, likely wait on hold, and ask your question to staff, or – if you’re tight on time – you just forget about it and hope for the best – something that’s not only frustrating but could potentially be detrimental to your health.
This is what happens when you use basic platforms that only support hard-coded “two-way” messaging and do not offer live staff support when patient inquiries stray. If patients are not able to seamlessly connect with live staff via text when necessary, it creates more hassle for the patient AND your call center. Think about it: Does your call center or front desk staff even have the resources to handle these extra calls that will come in as a result of unanswered texts?
With the Artera platform, you get two great options to make this better for your patients. For those that ultimately choose to dial in, if time is of the essence, our call-to text feature can easily transfer them to a text-enabled line for fast response. In fact, one customer using call-to-text decreased call abandonment rates by 25% or nearly 1,000 calls per month.
This response can be an automated prebuilt conversation or our staff console is available for live staff intervention when necessary – something that is used a tremendous amount. In fact, Artera’s staff console allowed health systems to engage 2.4 million unique patients4 via manual messages in a year. Without the console, that’s a minimum of 2.4 million phone calls, which translates to a potential $19M in added expenses (averaging $8-20 per call).
Even beyond the added efficiencies and cost savings, the staff console helps to keep the “human touch” alive in healthcare, allowing staff to respond in their own words and even emojis.
#8: Speak Your Patients’ Language
Nothing is more frustrating than needing help and the person who you’re speaking to for help doesn’t understand what you’re trying to say. Unfortunately, this happens all too often in health care – a widespread issue that creates barriers for patients to access the care they need.

According to a 2020 study, 67% of limited English speakers note language as a barrier to accessing care in the U.S., leading to poorer quality and outcomes. Several risk factors manifest in routine communication failures, such as instructions for medication or follow-up care questions.
Basic patient communication platforms that typically only provide limited language capabilities may not be able to reach a provider’s entire diverse population. If your patient population speaks additional languages or may not have English as their primary language, you’ll serve them better by engaging them in their preferred language. This reduces language barriers potentially hindering patients from receiving the care they may need and, therefore, resulting in poorer outcomes.
With Artera, you can speak your patients’ language. The Artera platform offers extended languages to send communications in 109+ different languages, increasing access to care and the ability to reach patients in their preferred languages. Languages include English, Spanish, Russian, Vietnamese, Korean, Arabic, Chinese, and many of the most common languages spoken in the US.
#9: Utilize Intelligent Analytics to Make Informed Decisions
If you’re reading this, your organization is likely increasing its investment in healthcare technology and digital solutions. What this also likely means is developing a greater understanding of how the tools you’re investing in are creating an impact across your organization and if there are opportunities to improve upon.
Did you know that Approximately 30% of the world’s data volume is generated by the healthcare industry today?
Regardless of your organization’s size or data capabilities, data insights will provide value to your entire organization. And in today’s world, your decisions – especially in regards to the patient experience – should be driven by data. So, what if you don’t have the ability to see any data through your new technology? How do you know if the platform is working? How do you make informed decisions to improve the patient experience?
That’s the reality of using some basic communication platforms that do not offer analytics capabilities – you DON’T have the ability to see data that can help inform your decisions to ultimately improve the patient experience and retain patients within your system. Without analytics, how can you expect to see what’s working and what isn’t working? How do you know your patients are truly happy with your communications strategy?
A strong analytics offering gets you the data you need, easily and seamlessly and delivers insights to help you see where improvements may be possible. With Artera, healthcare organizations receive analytics reports and dashboards that elevate reporting capabilities, power unique insights, and improve data value and transparency. You have the flexibility to use common reports that have helped more than 500 customers or you can create your own. Either way, you’ll have your data, your way.
Our customers have indicated that they love the Analytics dashboards and reports that are available to them: in fact, 100% of enterprise organizations that have Artera Analytics Plus utilize it every month.
Why settle for basic texting, when you can deliver better conversations with Artera?
Your patients deserve the best, so what are you waiting for? With better conversations comes better connections and even better outcomes. Learn how Artera fuels better conversations, here.
###
- Artera Data evaluating 16+ million patients, 2023
- 60+ million unique patient records, Artera Database, 2023
- Artera Data, 12-month average, 2023
- Artera Data from 940,000-patient health system, 2023


